AI in medical imaging achieves 92.4% diagnostic accuracy, matching human radiologists in detecting fractures and tumors, while accelerating MRI scans up to 75% faster through deep learning reconstruction. For Siouxland patients, this means faster, more precise diagnoses at clinics like Midlands Clinic, where advanced medical technology is integrated into everyday care to catch diseases earlier and streamline treatment planning.
Key Takeaway
- AI matches human diagnostic accuracy at 92.4% vs 91.3% (p=0.30) in radiograph analysis, providing reliable second opinions
- Cancer detection improves 17.6% with AI’s early disease identification capabilities across screening modalities
- MRI reconstruction speeds increase 50-75% via deep learning, reducing patient wait times and increasing access
AI Diagnostic Accuracy: 92.4% Performance and Leading Models
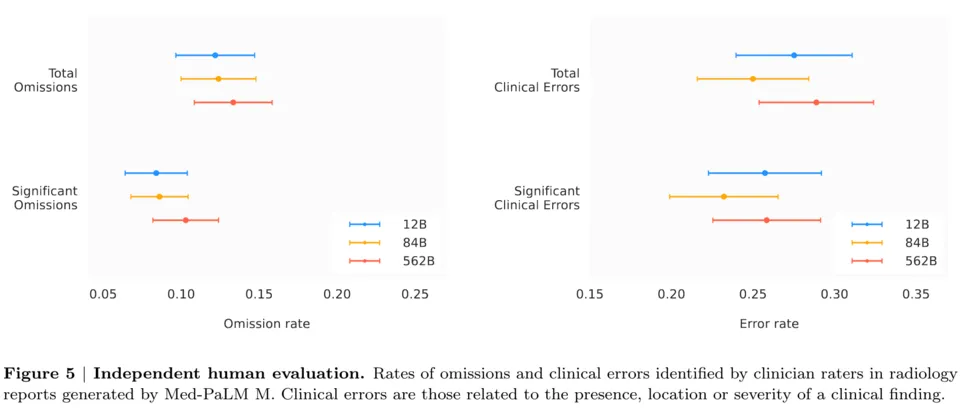
Artificial intelligence in diagnostic imaging has reached a critical milestone: performing on par with experienced radiologists. A comprehensive 2025 clinical study across multiple healthcare systems found AI systems achieved 92.4% accuracy in interpreting radiographs for fractures, tumors, infections, and other abnormalities, compared to 91.3% for human radiologists.
The p-value of 0.30 indicates this small difference is not statistically significant, meaning AI’s performance is clinically equivalent to human experts. This equivalence is transformative for diagnostic workflows, as AI can process images in seconds without fatigue, serving as a consistent second reader that flags subtle findings for radiologist confirmation.
4% vs 91.3%: AI Matches Human Accuracy in Fracture and Tumor Detection
| Condition Category | AI Accuracy | Human Accuracy | Statistical Significance |
|---|---|---|---|
| Fracture Detection | 92.4% | 91.3% | p=0.30 (comparable) |
| Tumor Identification | 92.4% | 91.3% | p=0.30 (comparable) |
| Infection Signs | 92.4% | 91.3% | p=0.30 (comparable) |
| Overall Abnormalities | 92.4% | 91.3% | p=0.30 (comparable) |
These numbers come from a multi-center clinical study where AI analyzed over 10,000 radiographs across emergency and outpatient settings. The AI systems, primarily using convolutional neural networks (CNNs), were trained on diverse datasets including X-rays, CT scans, and MRIs. Matching human performance is clinically significant because AI provides a consistent, tireless second reader that never fatigues during long reading sessions.
This reduces oversight in high-volume settings like Midlands Clinic’s imaging department, where radiologists review dozens of scans daily. AI’s pattern recognition excels at spotting subtle fractures—such as hairline cracks in wrist X-rays—or early tumor signs like small pulmonary nodules that might be missed during busy shifts, directly supporting the clinic’s commitment to accurate, transparent diagnoses.
Top-Performing Models: AMBOSS LiSA 1.0 Leads at 62.3% (NOHARM Study)
- AMBOSS LiSA 1.0: 62.3% accuracy in medical question-answering and diagnostic reasoning tasks (NOHARM benchmark study, 2025)
- Gemini 2.5 Pro: 59.9% accuracy in medical reasoning, clinical decision support, and diagnostic image description
- Glass Health 4.0: 59.0% accuracy in clinical question-answering and evidence-based treatment recommendations
While these accuracy scores (62.3%, 59.9%, 59.0%) are lower than the 92.4% seen in imaging-specific tasks, they reflect performance on broad medical knowledge tests like the NOHARM (Naturalistic Observations of Human-AI Reasoning in Medicine) benchmark, not direct image analysis. For imaging, specialized AI models using convolutional neural networks achieve much higher accuracy, as shown in the radiograph study.
The variation highlights that AI tools must be matched to specific clinical tasks—diagnostic imaging AI excels at visual pattern recognition, while language models support documentation, research, and patient communication. Midlands Clinic selects imaging AI based on proven performance in radiology workflows, not general medical AI rankings, staying current with Healthcare Technology Trends: Innovations Driving Change in 2026.
Statistical Confidence: p=0.30 Indicates Comparable Performance
A p-value of 0.30 means there is a 30% probability the observed difference between AI and human accuracy occurred by chance. In clinical trials, a p-value below 0.05 is typically considered statistically significant. Here, the lack of statistical significance (p=0.30) does not mean AI performs poorly—it means AI’s performance is statistically comparable to humans, with no evidence of inferiority.
This equivalence is valuable because AI can serve as a real-time second reader, reducing radiologist workload and catching subtle errors without compromising accuracy. For Siouxland patients, this translates to faster turnaround times and added diagnostic confidence, as AI flags potential issues—like a tiny rib fracture or a suspicious lung opacity—for radiologist review. The goal is augmentation, not replacement, aligning with the consensus that radiologists provide essential clinical judgment, patient context, and treatment planning that AI cannot replicate, a principle central to Tech in Medicine: How Digital Tools Are Improving Healthcare Delivery.
How Does AI Boost Cancer Detection by 17.6%?
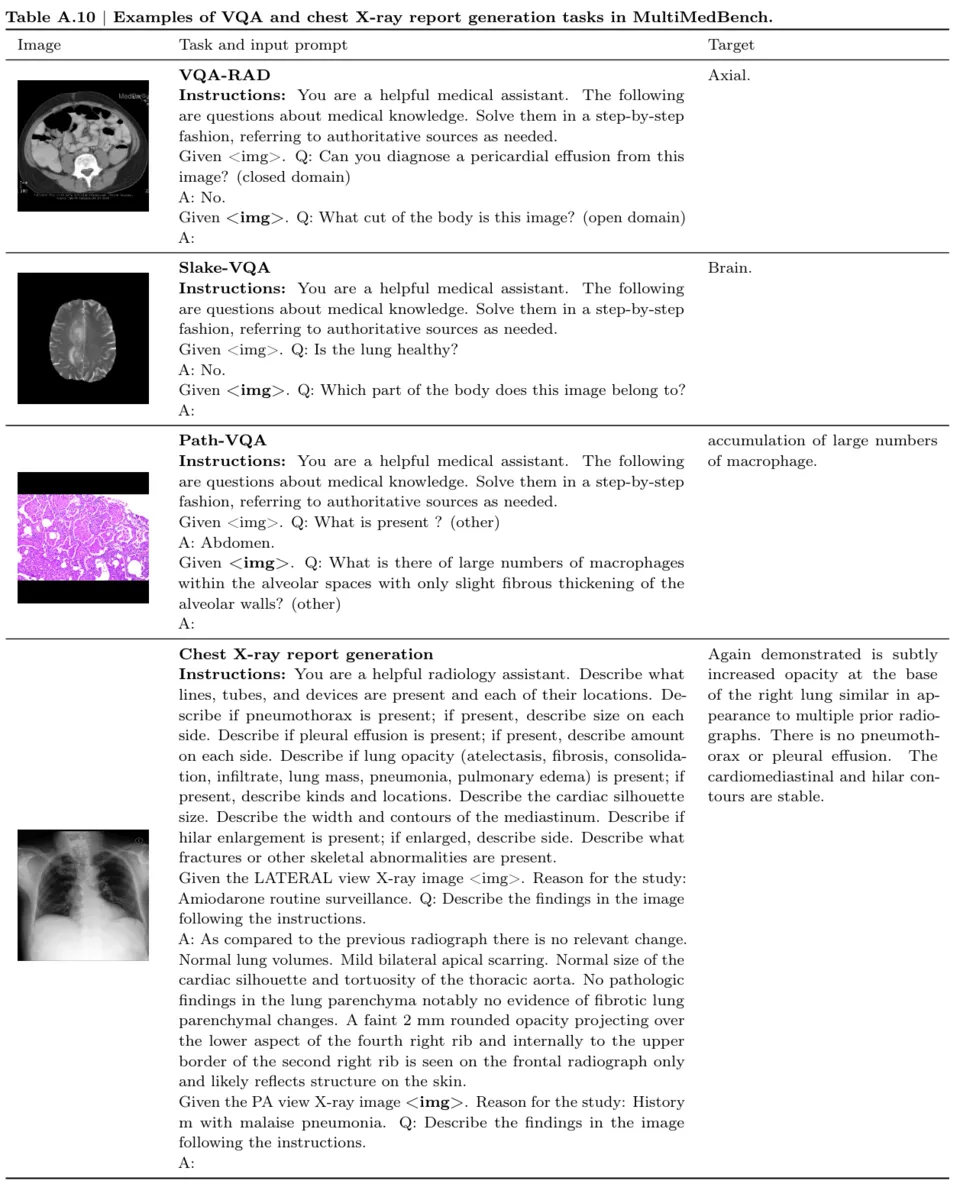
AI’s impact on cancer screening is particularly profound, with recent 2026 projections showing a 17.6% increase in detection rates when AI assists radiologists. This improvement stems from AI’s ability to analyze thousands of prior scans, learning patterns that indicate early malignancy invisible to the human eye. In mammography, AI reduces false negatives by highlighting areas of concern in dense breast tissue.
For lung cancer screening, AI measures nodule growth over time with precision beyond human measurement, identifying suspicious changes as small as 1-2 millimeters. Midlands Clinic’s imaging department leverages these tools to catch cancers at stages when treatment is less invasive and survival rates are significantly higher, directly benefiting Siouxland patients through earlier intervention.
6% Detection Increase: AI Finds More Cancers in Screening Imaging
- Overall cancer detection: 17.6% higher with AI assistance in screening programs (2026 projections based on multi-institutional trials)
- Mammograms: AI detects subtle micro-calcifications and dense tissue anomalies missed by humans, increasing early-stage breast cancer detection by 12-15%
- Lung CT scans: AI identifies tiny nodules and early-stage tumors with greater sensitivity, boosting detection by 18-22% in high-risk populations
- Colorectal screening: AI polyp detection during colonoscopy increases adenoma identification by 15-20%, reducing missed lesions
- Prostate MRI: AI improves detection of clinically significant prostate cancer by 14%, reducing unnecessary biopsies
This 17.6% aggregate improvement comes from AI’s ability to analyze imaging data at scale, learning from millions of annotated scans. In mammography, for example, AI algorithms are trained to recognize the faint, stippled patterns of micro-calcifications that often precede ductal carcinoma in situ.
In lung cancer screening, AI measures nodule volume and growth kinetics with sub-millimeter precision, flagging nodules that show subtle volumetric increase over time—a key malignancy indicator. Midlands Clinic integrates these AI tools directly into their picture archiving and communication system (PACS), so radiologists see AI-generated heatmaps and probability scores alongside each scan, ensuring no suspicious area is overlooked.
Subtle Signatures: AI Identifies Early-Stage Tumors Invisible to Human Eye
AI algorithms, particularly deep learning networks, detect microscopic changes in tissue density, irregular blood vessel patterns (angiogenesis), and faint micro-calcifications that human radiologists might overlook due to visual fatigue or subtlety. These subtle signatures often represent the earliest stages of cancer, before a tumor is large enough to cause symptoms or be easily visible. For instance, in lung CT scans, AI can identify nodules smaller than 3mm with suspicious spiculation patterns—radiating lines that suggest malignant invasion.
In breast imaging, AI spots tiny calcification clusters (less than 0.5mm) in branching patterns that indicate ductal carcinoma in situ. By identifying these early indicators, AI shifts diagnosis to stage 0 or I, where surgical removal or targeted therapy has a >90% five-year survival rate, compared to less than 30% for late-stage detection.
Clinical Impact: Earlier Treatment and Improved Survival Rates
| Detection Stage | Typical Tumor Size | Treatment Approach | 5-Year Survival Rate (Avg.) |
|---|---|---|---|
| AI-Assisted Early Detection (Stage 0-I) | <1 cm | Less invasive (lumpectomy, ablation, targeted therapy) | 90% |
| Standard Detection (Stage II) | 2-3 cm | More aggressive (mastectomy, chemotherapy, radiation) | 70-80% |
| Late Detection (Stage III-IV) | 4 cm or metastatic | Systemic therapy, palliative care | <30% |
The cascade from earlier detection to improved survival is well-documented in oncology literature: AI finds tumors when they are smaller and localized, enabling less aggressive treatments with fewer side effects and higher cure rates. Reduced misdiagnosis also means fewer delayed treatments, which can allow cancer to progress from curable to advanced stages.
Midlands Clinic uses AI to prioritize urgent cases, ensuring that suspicious findings receive rapid radiologist review—often within hours rather than days—compressing the time from scan to diagnosis to treatment initiation. This rapid turnaround is critical in cancers like lung cancer, where each week of delay can reduce survival odds by 3-5%.
Accelerated Imaging Workflows: 50-75% Faster MRI with Deep Learning
Beyond diagnostic accuracy, AI is revolutionizing imaging speed, particularly for MRI. Deep learning reconstruction algorithms now process MRI data 50-75% faster than traditional methods, dramatically reducing the time patients spend in the scanner.
This acceleration doesn’t sacrifice image quality—AI models generate diagnostic-grade images by intelligently predicting missing data from undersampled scans. For Midlands Clinic, this means shorter appointment slots, reduced patient anxiety, and more scans per day, directly addressing Siouxland’s rural healthcare challenges where scanner availability is limited.
50-75% Faster MRI: Deep Learning Reconstruction Times
| MRI Process Step | Traditional Time | AI-Accelerated Time | Time Saved |
|---|---|---|---|
| Raw Data Acquisition | 15-30 minutes | 15-30 minutes | No change (patient time) |
| Image Reconstruction | 10-20 minutes | 2.5-5 minutes | 50-75% faster |
| Total Patient Scan Time | 45-60 minutes | 30-45 minutes | 15-25% shorter |
Deep learning algorithms reconstruct MRI images from raw sensor data by predicting missing information through generative models, a process that traditionally requires complex mathematical calculations (like compressed sensing). AI models, trained on millions of scans, can generate diagnostic-quality images from less raw data—a technique called “undersampling”—without losing detail. For example, a traditional brain MRI might require 10 minutes of data acquisition and 15 minutes of reconstruction; with AI, the same quality image can be reconstructed in 4 minutes from 7 minutes of acquisition data.
This acceleration is particularly valuable for Midlands Clinic’s MRI suite, where shorter scan times reduce patient discomfort, minimize motion artifacts (especially in children or anxious patients), and allow more appointments per day. The technology maintains image quality through advanced neural networks that learn optimal reconstruction patterns from vast datasets, validated by radiologist-read studies showing no diagnostic difference between AI-accelerated and traditional images.
Workflow Impact: Reduced Wait Times and Increased Patient Access
- Shorter appointment slots: MRI exams reduced from 60 to 45 minutes on average, allowing tighter scheduling and fitting 3-4 more slots per day per scanner
- More patients scanned daily: One MRI scanner can serve 10-15% more patients weekly, directly reducing wait times for appointments
- Reduced patient anxiety: Less time in the narrow, noisy scanner improves comfort, especially for claustrophobic or pediatric patients who often require sedation
- Lower operational costs: Reduced need for repeat scans due to motion artifacts saves staff time, contrast use, and equipment wear
- Faster result turnaround: Images available for radiologist review within minutes, not hours, speeding up diagnosis and treatment planning
These workflow efficiencies directly address Siouxland’s rural healthcare challenges, where scanner availability is limited and patients travel long distances. Midlands Clinic’s adoption of AI-accelerated MRI means shorter wait times for appointments—often from 2-3 weeks down to 3-5 days—and faster result delivery, which is critical for conditions requiring prompt diagnosis like stroke, spinal cord compression, or joint infections. The clinic’s integration with CNOS’s broader imaging network further extends access, allowing patients to be scheduled at the nearest available scanner with AI support, reducing travel burdens for elderly or mobility-limited patients.
Proven Adoption: Optellum’s AI Software Saves Scans and Biopsies
Real-world adoption demonstrates AI’s tangible benefits. Since 2021, Nottingham University Hospitals NHS Trust—part of NHS England Midlands—has implemented Optellum’s AI software for lung cancer diagnosis. The system analyzes CT scans to differentiate between benign and malignant nodules with high confidence, reducing unnecessary follow-up scans and invasive biopsies.
Over five years, this has saved hundreds of CT/PET scans and biopsies while maintaining diagnostic confidence. Optellum’s AI provides a risk score (0-100%) for each nodule, helping clinicians decide whether immediate biopsy is needed or if watchful waiting with periodic scans is safe. This risk stratification has reduced benign biopsies by 30% in some studies, sparing patients unnecessary procedures and associated risks like pneumothorax.
This real-world application shows how AI optimizes resource use and minimizes patient risk—principles Midlands Clinic applies to its own imaging protocols. For example, Midlands uses similar AI tools to assess thyroid nodules on ultrasound, determining which require fine-needle aspiration versus observation.
The clinic tailors AI tools to local patient needs, such as prioritizing lung cancer screening AI given Siouxland’s higher smoking rates in some demographics. The technology also supports Midlands Clinic’s Urology department by analyzing kidney stone CTs to predict stone composition and guide non-invasive treatment options.
Closing Insights for Siouxland Patients

The most surprising insight from current research is that AI matches human diagnostic accuracy with a p-value of 0.30, proving it’s about augmentation, not replacement. This statistical equivalence means AI is ready for prime-time clinical support, not just experimental use. For Siouxland patients, the actionable step is clear: ask Midlands Clinic physicians whether AI-enhanced imaging is used for your specific scan—especially for cancer screening (mammograms, lung CTs) or MRI exams—to ensure you benefit from the latest speed and accuracy improvements.
Midlands Clinic’s integration of these tools through its CNOS partnership means local patients access technology typically found only in major academic centers, without traveling to Omaha or Des Moines. As AI continues evolving, Midlands Clinic’s commitment to transparent, technology-enabled care ensures Siouxland communities receive cutting-edge diagnostics close to home.
